Prostate health is an important issue that requires regular follow-up, especially with advancing age. Complaints such as difficulty urinating, frequent urination, or waking up at night to urinate may arise for different reasons, and reliable tests are needed for an accurate evaluation. At this point, prostate screening tests help both determine the level of risk and clarify the source of the symptoms. A screening approach planned individually by a urology specialist helps reduce unnecessary anxiety while ensuring the right steps are taken on time.
Why Are Prostate Screening Tests Important?
Prostate health is an issue that should be monitored more closely in men as they age. Over time, benign enlargement, inflammation, or in some cases malignant changes may occur in the prostate tissue. At this point, prostate screening tests help both identify the source of the problem in patients with symptoms and detect possible issues at an early stage in individuals within certain risk groups. The screening and evaluation approach is individualized; age, family history, current complaints, and examination findings are all considered together.
The aim of a urological check-up is not to make a definitive diagnosis with a single test, but to determine the right course of action by bringing together different findings. For this reason, prostate screening tests should be considered as a whole. Some tests are used more for risk assessment, some show how the urinary system is functioning, and others provide information about the anatomical structure of the bladder and prostate. When the appropriate combination is selected, unnecessary anxiety is reduced and clearer, faster steps can be taken when needed.
PSA
PSA is a blood parameter known as “Prostate-Specific Antigen.” In daily practice, it is one of the best-known prostate screening tests. PSA alone is not an indicator of cancer; it is a value related to prostate tissue and may become elevated in different situations. For example, benign prostate enlargement, prostate inflammation (prostatitis), some recent infections, and even certain procedures affecting the prostate may change the PSA value. Therefore, the PSA result should always be evaluated together with the person’s age, prostate volume, symptoms, and physician examination findings.
In PSA assessment, it is not enough to view the result simply as high or normal. In some patients, the rate of change over the years, and in others, additional parameters or ratios such as free PSA, may influence clinical decisions.
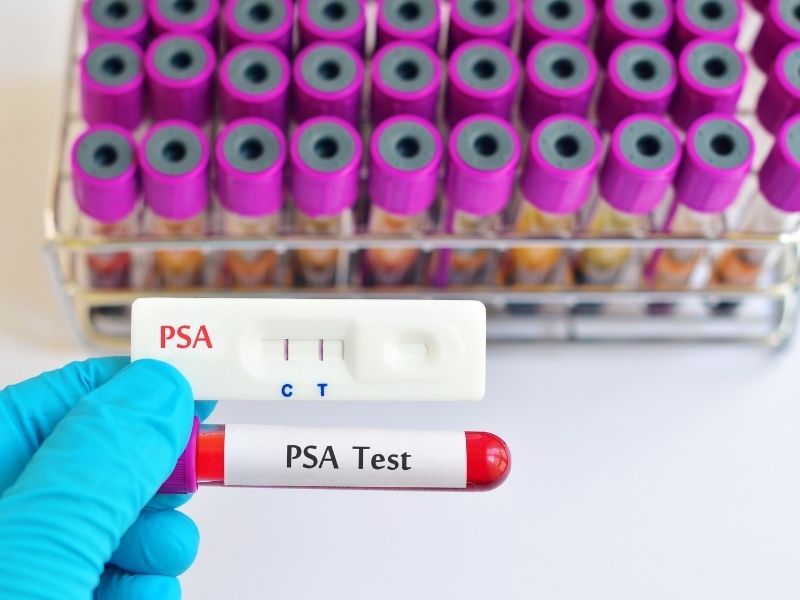
The main aim of the urology examination is to place the PSA result in the correct clinical context. This approach can reduce unnecessary advanced investigations within the scope of prostate screening tests while also helping distinguish more clearly the patients who truly require closer follow-up.
Urinalysis
Although it may seem simple, urinalysis is a very valuable step in urological evaluation. Within prostate screening tests, the role of urinalysis is important especially for detecting clues related to urinary tract infection, bleeding (hematuria), signs of inflammation, the presence of crystals, and some findings that may indirectly suggest kidney function issues. Complaints related to the prostate often overlap with the urinary tract; symptoms such as frequent urination, burning, difficulty urinating, and waking up at night to urinate may not always be caused by the prostate alone.
For this reason, urinalysis works like a screening step that helps clarify the background of the complaint. In some cases, additional tests such as urine culture may also be necessary. Especially in patients with suspected infection, the interpretation of many findings, including PSA assessment, may change. Therefore, urinalysis is often accepted as one of the first steps in the prostate screening test approach.
Voiding Test: Uroflowmetry
Uroflowmetry is a practical test that measures the speed of urination and the voiding pattern. The patient urinates into a special device, and the device records the maximum flow rate, average flow rate, and duration of urination. Among prostate screening tests, uroflowmetry is especially helpful in cases with complaints such as weak urine flow, interrupted urination, prolonged waiting time before urination, and a feeling of incomplete emptying.
Uroflowmetry alone does not establish whether prostate enlargement is present or not; however, it provides objective data on how comfortably the urinary tract is functioning. In some patients, this test may also be valuable for monitoring the response to treatment. For example, changes in flow rate after medication or the objective counterpart of symptoms can be followed through uroflowmetry. In this respect, uroflowmetry is an important part of prostate screening tests that strengthens the functional evaluation.

Ultrasonography
Ultrasonography is a frequently used imaging method in the anatomical evaluation of the prostate and urinary tract and does not involve radiation. Within the scope of prostate screening tests, ultrasound may help assess prostate volume, the bladder wall, whether there is dilation in the kidneys, and how well the bladder empties (post-void residual urine volume). Especially in patients who feel unable to empty completely, seeing the amount of urine remaining in the bladder provides meaningful clues for treatment planning.
The ultrasound approach may vary from person to person. In some patients, an abdominal ultrasound is sufficient, while in other cases more detailed methods such as transrectal ultrasound may be considered. Knowing the prostate volume allows a more accurate interpretation when it is correlated with symptoms. For this reason, ultrasound can make both risk assessment and the possible mechanism of symptoms more visible within the overall prostate screening test approach.
Cystoscopy
Cystoscopy is an endoscopic procedure in which the urethra and bladder are evaluated directly by visualization. Within prostate screening tests, cystoscopy is not a routine screening test performed in every patient; rather, it is used in selected situations to clarify the cause of specific complaints. For example, the physician may consider cystoscopy in cases such as blood in the urine, recurrent urinary tract infections, severe lower urinary tract symptoms, suspected narrowing of the urethra, or the possibility of a structural problem inside the bladder.
With cystoscopy, observational information can be obtained about the inner surface of the bladder, the bladder neck, the course of the urethra, and whether the prostate is compressing the urinary canal. Thanks to this procedure, the source of complaints can be understood more clearly in some patients, and unnecessary treatment trials can be reduced. When performed with the correct indication, cystoscopy becomes one of the important steps within the prostate screening test approach that helps clarify the diagnosis.